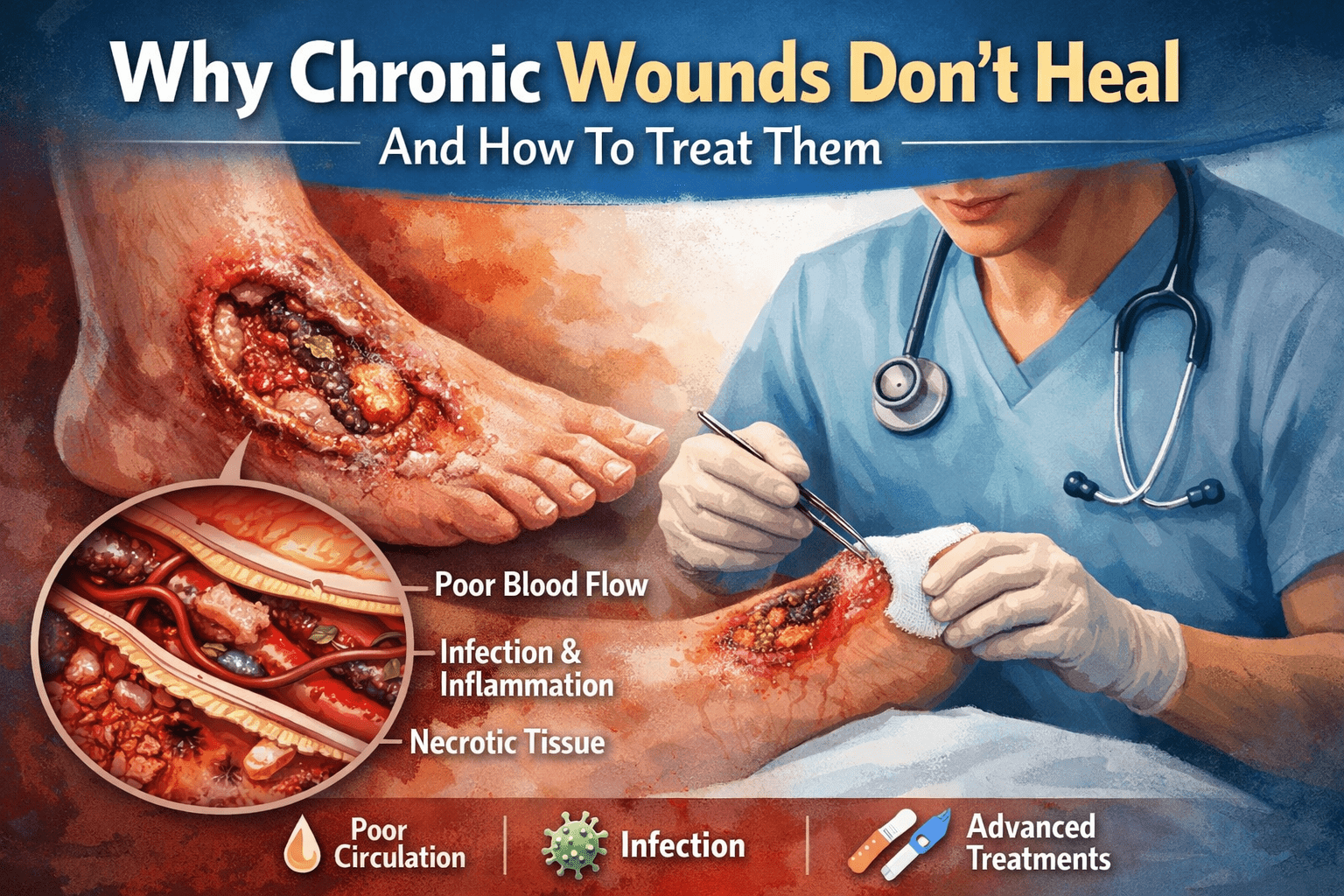
As our population ages, chronic wounds are becoming one of the most overlooked health challenges facing older adults. Limited mobility, diabetes, vascular disease, and fragile skin make seniors especially vulnerable to slow-healing wounds that can quickly escalate into serious complications.
Mobile wound care services are transforming how elderly patients receive treatment by delivering advanced wound management directly to the home. Instead of navigating transportation barriers, long clinic waits, and hospital exposure risks, seniors receive expert evaluation, treatment, and monitoring where they are most comfortable.
This model improves outcomes, reduces hospitalizations, and restores dignity for elderly patients who deserve specialized, compassionate support.
The Growing Need for Mobile Wound Care in the Elderly Population
Chronic wounds affect millions of older adults each year. Conditions such as diabetes, peripheral artery disease, immobility, and malnutrition increase the risk of pressure injuries, diabetic foot ulcers, venous leg ulcers, arterial ulcers, and post-surgical wounds.
For seniors, a wound is rarely “just a wound.” Delayed healing can lead to infection, sepsis, amputation, and hospitalization.
Traditional clinic-based wound care presents challenges including transportation limitations, caregiver burden, increased fall risk during travel, exposure to hospital-acquired infections, and missed follow-up appointments.
Mobile wound care eliminates these barriers by delivering consistent, specialized treatment in the home environment.
What Is Mobile Wound Care and How It Works
Mobile wound care is a healthcare service where wound care specialists travel to patients’ homes, assisted living facilities, or skilled nursing environments to provide evaluation and treatment.
Services typically include comprehensive wound assessment, debridement procedures, advanced dressings, infection management, negative pressure wound therapy, biologic or skin substitute applications, and care coordination with primary providers.
Mobile clinicians often collaborate with primary care physicians, home health agencies, and specialists to ensure continuity of treatment.
Instead of episodic clinic visits, mobile wound care offers structured, ongoing management that adapts to the patient’s healing progress.
Common Wounds Treated in Elderly Patients
Older adults face unique wound types due to physiological changes and chronic conditions.
Pressure Injuries
Pressure injuries develop from prolonged pressure on bony areas such as the heels, hips, or sacrum. Limited mobility, bed rest, and frailty increase risk. Early detection and skilled wound staging are essential to prevent deep tissue damage and long-term complications.
Diabetic Foot Ulcers
Diabetes impairs circulation and sensation, making small foot injuries dangerous. Without timely intervention, diabetic ulcers can become infected or lead to amputation. Mobile wound specialists provide routine monitoring, debridement, and advanced therapies to support limb preservation.
Other commonly treated wounds include venous leg ulcers, arterial ulcers, skin tears, traumatic wounds, and post-surgical incisions that require ongoing supervision.
Benefits of Receiving Wound Care at Home
Mobile wound care offers both clinical and emotional advantages for elderly patients.
Reduced Hospitalizations
Timely wound monitoring and early infection detection reduce emergency room visits and hospital admissions. Proactive intervention prevents minor issues from escalating into life-threatening complications.
Improved Healing Compliance
Patients are more likely to adhere to treatment plans when care is convenient and consistent. Home-based education empowers seniors and caregivers to participate actively in wound management and follow prescribed protocols correctly.
Enhanced Comfort and Dignity
Healing at home reduces stress, anxiety, and fatigue. Elderly patients maintain independence and avoid the physical strain of transportation.
Home-based care also allows clinicians to assess environmental factors, nutrition, fall risks, and mobility challenges that directly impact wound healing outcomes.
Advanced Technologies Used in Mobile Wound Care
Modern mobile wound care services bring hospital-level tools directly into the home setting.
Negative Pressure Wound Therapy
Also known as wound vacuum therapy, negative pressure wound therapy promotes healing by removing excess fluid and improving circulation at the wound site. Portable systems make this therapy accessible outside hospital environments, increasing treatment accessibility for elderly patients.
Biologic Dressings and Skin Substitutes
Advanced wound products such as collagen dressings, growth factor treatments, and bioengineered skin substitutes accelerate tissue regeneration in chronic wounds that have stalled in the healing process.
Digital Wound Monitoring
Some providers use digital imaging and measurement technology to track wound size, depth, and healing progress objectively. This data-driven approach improves clinical decision-making and ensures timely treatment adjustments.
Mobile wound care is no longer limited to basic dressing changes. It is comprehensive, technology-supported treatment delivered with precision.
The Role of Caregivers in Mobile Wound Healing
Caregivers play a vital role in wound recovery for elderly patients, especially those with mobility limitations or cognitive decline.
Mobile wound care teams often provide dressing change training, infection warning sign education, nutritional guidance, and offloading or repositioning instruction to reduce pressure injuries.
When caregivers understand the wound care plan and receive proper training, healing outcomes improve significantly.
Home-based clinicians can also evaluate pressure surfaces, assistive devices, and daily routines that may affect recovery. This broader assessment rarely occurs during brief outpatient visits.
Preventing Complications in Elderly Wound Care
Prevention remains as important as treatment.
Key strategies include routine skin assessments, proper offloading techniques, blood sugar management, adequate hydration, sufficient protein intake, and early infection intervention.
Elderly skin is thinner and more fragile, increasing susceptibility to breakdown. A mobile wound care provider can identify early warning signs before wounds worsen.
Preventative mobile visits are especially valuable for high-risk patients with diabetes, vascular disease, or limited mobility.
Choosing the Right Mobile Wound Care Provider
Selecting a qualified mobile wound care service is essential for achieving optimal healing outcomes.
Look for providers who offer board-certified wound specialists, experience with geriatric patients, access to advanced treatment modalities, coordinated communication with physicians, and clear documentation practices.
Mobile wound care requires specialized training and a structured clinical approach. It should not be treated as a convenience service alone, but as a critical extension of the healthcare system for elderly patients.
The Future of Elderly Wound Care Is Mobile
Healthcare is steadily shifting toward patient-centered, home-based models that reduce hospital dependency and improve quality of life for seniors.
Mobile wound care represents this evolution by combining advanced medical technology, specialized expertise, and compassionate in-home support. It allows elderly patients to heal in a familiar environment while receiving structured, evidence-based treatment.
For families, it means fewer emergency visits, lower stress, and confidence that their loved one is receiving professional care without unnecessary disruption.
For seniors, it means healing with dignity and safety.
And honestly, if we can deliver groceries, prescriptions, and physical therapy to someone’s door, delivering advanced wound treatment should not feel like innovation. It should feel like common sense.
Frequently Asked Questions
What types of wounds qualify for mobile wound care services?
Mobile wound care services treat most chronic and non-healing wounds in elderly patients. This includes pressure injuries, diabetic foot ulcers, venous leg ulcers, arterial ulcers, post-surgical wounds, and traumatic skin tears. A licensed wound care specialist evaluates the wound’s severity, infection risk, and healing stage to determine eligibility and create a customized treatment plan at home.
Is mobile wound care covered by Medicare?
Medicare often covers medically necessary mobile wound care services when ordered by a physician and properly documented. Coverage typically includes wound assessments, debridement, advanced dressings, and certain therapies. Eligibility depends on diagnosis, medical necessity, and compliance with Medicare guidelines. Supplemental insurance may reduce out-of-pocket costs for eligible elderly patients.
How often will a mobile wound care specialist visit?
The frequency of mobile wound care visits depends on wound severity, infection risk, and healing progress. Many elderly patients receive weekly visits, while complex or infected wounds may require multiple visits per week. As healing improves, visit frequency is adjusted based on clinical evaluation and documented progress.
When should I seek professional wound care for an elderly loved one?
Seek professional mobile wound care if a wound does not improve within 10 to 14 days, increases in size, becomes red or swollen, produces drainage, or causes pain. Immediate evaluation is especially important for seniors with diabetes, poor circulation, or limited mobility to prevent infection and serious complications.