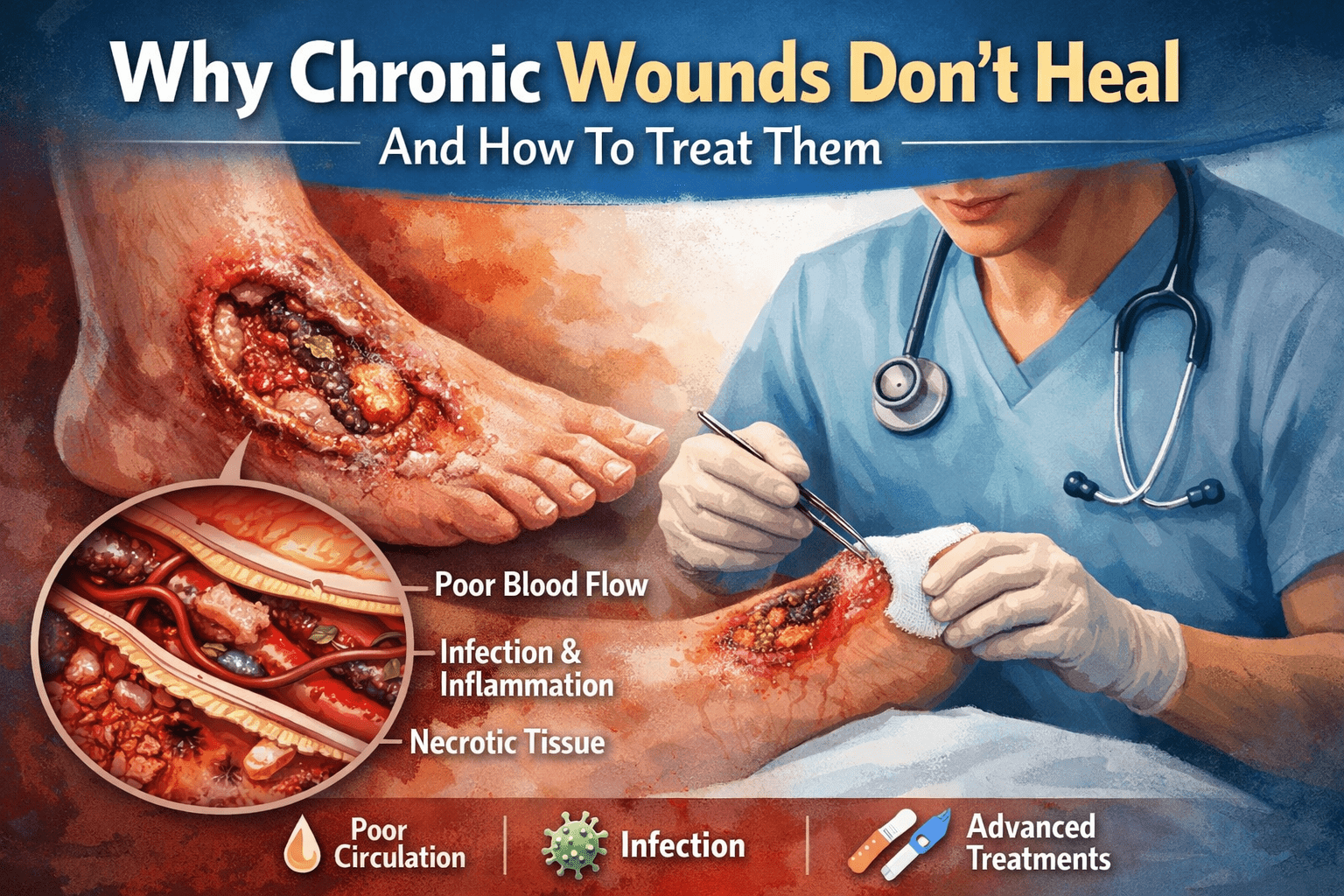
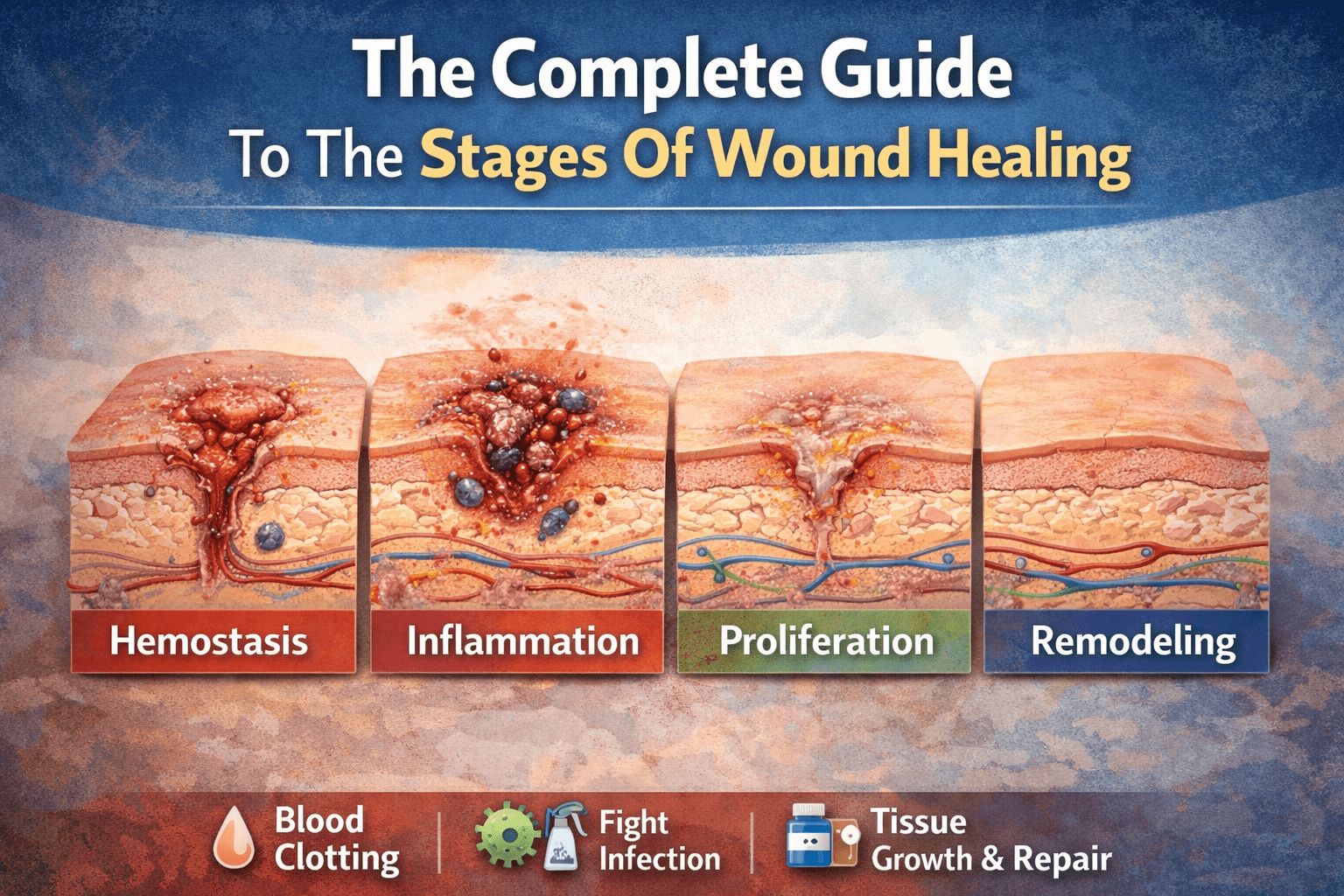
A simple wound can look harmless in the morning and concerning by evening. Healing is not just about covering it and hoping for the best. It is about creating the right conditions for the body to repair itself safely.
Have you ever wondered if you are cleaning a wound properly? Or if changing a dressing too often could actually slow healing? Many caregivers worry about doing too much or too little.
Here is why caution matters. According to the Centers for Disease Control and Prevention, one in 31 hospital patients has at least one healthcare-associated infection on any given day. Germs spread through unclean hands or improperly handled equipment remain one of the leading causes of preventable infection. That statistic alone shows how critical hygiene and proper wound management truly are.
The good news is that following structured, evidence-based wound care tips significantly lowers risk. When caregivers understand tips for hygienic wound care, safe dressing changes at home, and early signs of wound infection, healing becomes more predictable and far less stressful.
At Inspiring Minds Wound Care, we support families every day with practical guidance and advanced wound care in Ohio when needed.
In this article, we will walk through essential wound care tips and tricks, elderly wound care tips for fragile skin, pressure sore prevention strategies, preventing wound infection through proper hygiene, and when to call a wound specialist before complications arise.
“Healing at home requires structure, vigilance, and the right support. Inspiring Minds Wound Care helps caregivers protect recovery with expert guidance and timely intervention when it matters most.”

How To Practice Safe And Hygienic Wound Care At Home
When it comes to caring for wounds at home, hygiene is not optional. It is the foundation of healing. Most wound complications begin with simple contamination, not complex medical failure.
If you focus on nothing else, focus on cleanliness.
According to the CDC, germs that cause healthcare-associated infections often spread through unclean hands or improper handling of equipment. That same risk exists in the home setting. This is why strong home wound care safety habits matter every single time you change a dressing.
Let’s break this down into simple, manageable steps.
1. Create A Clean Zone Before You Begin
Do not change a dressing wherever it feels convenient.
Choose a flat, well-lit surface. Wipe it down with disinfectant. Lay down a clean barrier such as a fresh towel or disposable medical pad.
Keep pets away. Turn off fans that may blow dust. Small details reduce contamination risk.
One helpful method we teach families is the “prepare before you expose” rule. Have every supply opened and ready before you uncover the wound. The less time the wound is exposed to air, the better.
2. Wash Hands The Right Way Every Time
Tips for hygienic wound care always begin with handwashing.
Wash your hands with soap and water for at least 20 seconds. Dry them with a clean towel. Then apply disposable gloves.
Gloves are not a replacement for handwashing. They are a second layer of protection.
Remove jewelry and watches before starting. Bacteria hide under rings more than people realize.
3. Clean The Wound Gently And Correctly
When cleaning the wound:
- Use sterile saline whenever possible
- Clean in a circular motion from the center outward
- Avoid scrubbing aggressively
- Never use hydrogen peroxide or alcohol unless directed by a clinician
Harsh chemicals may kill bacteria, but they also damage healthy cells trying to rebuild tissue.
Safe dressing changes at home require balance. You want to remove debris without harming new growth.
4. Handle Dressings With Care
Before placing a new dressing:
- Inspect the wound for changes
- Check surrounding skin for redness or breakdown
- Confirm there is no unusual odor
Dispose of used dressings immediately in a sealed plastic bag. Do not leave them on countertops.
If a dressing sticks, never pull it off dry. Moisten it with saline and allow it to release naturally. Protecting fragile tissue prevents setbacks.
5. Follow The Hygiene Hierarchy
Think of wound care as a four-level system:
Level 1: Clean Environment
Level 2: Clean Hands
Level 3: Clean Tools
Level 4: Clean Wound Handling
If one level breaks down, infection risk increases.
Practicing structured wound care tips like these dramatically lowers the chances of complications and supports smoother healing.
Strong hygiene routines reduce the risk before it begins. That is why professional wound care teams emphasize cleanliness first, dressings second.
If you ever notice increasing redness, drainage changes, or warmth around the wound, those may be early signs of wound infection and should not be ignored.
Hygiene protects progress. Consistency protects recovery.
Manage Complex Wounds With Experts Care
At Inspiring Minds Wound Care, we work closely with caregivers to ensure wounds are healing properly. Our team provides clinical assessment, advanced treatment options, and ongoing guidance tailored to each patient’s needs.
How To Perform Safe Dressing Changes At Home
Changing a dressing is more than removing a bandage and putting on a new one. It is your opportunity to assess healing, prevent infection, and protect new tissue.
Many caregivers worry about doing it wrong. The truth is, most problems happen when dressing changes at home are rushed or done without preparation.
Let’s slow it down and make it structured.
1. Prepare Everything Before Removing The Old Dressing
Never uncover the wound and then start searching for supplies.
Before you begin:
- Wash your hands thoroughly
- Lay out sterile gauze, saline, gloves, and new dressings
- Have a disposal bag ready
- Ensure the room is warm and well lit
When the wound is exposed, its temperature drops quickly. Research shows that wound cells function best at normal body temperature, and repeated cooling during dressing changes at home can slow tissue repair.
Preparation reduces exposure time and protects healing.
2. Remove The Old Dressing Gently
If the dressing lifts easily, remove it slowly and carefully.
If it sticks, do not pull.
Soak the area with sterile saline and allow the bandage to loosen naturally. Pulling dry gauze can tear fragile new tissue, setting healing back several days.
This is one of the most overlooked wound care tips and tricks. Protecting new tissue matters more than speed.
3. Assess The Wound Every Time
Each dressing change is a checkpoint.
Look for:
- Reduction in wound size
- Healthy pink or red tissue
- Balanced moisture
- Changes in drainage
Also watch for early signs of wound infection such as spreading redness, thick discharge, unusual odor, or increasing pain.
Taking a photo every three days can help you objectively track progress. Healing can feel slow, but visual comparison often shows improvement you might otherwise miss.
4. Choose The Right Dressing For The Wound Type
Not all dressings serve the same purpose. Here is a simple guide:
Hydrogel: Best for dry wounds, adds moisture.
Foam: Ideal for wounds with moderate drainage, absorbs fluid.
Transparent film: Useful for minor wounds, allows visibility.
Calcium alginate: Designed for heavy drainage, forms a protective gel.
The goal is moisture balance. Modern healing works best when wounds are moist but not soaked. Too dry slows repair. Too wet damages surrounding skin. Understanding this balance is one of the most valuable wound care tips for caregivers.
5. Secure The Dressing Without Damaging Skin
Be mindful when applying adhesive. Especially in elderly patients, skin tears easily. Avoid aggressive tapes. Consider silicone-based adhesives when possible.
Press gently. Do not stretch the skin. These small adjustments support both elderly wound care tips and overall home wound care safety.

Elderly Wound Care Tips For Fragile Skin
As we age, skin changes dramatically. It becomes thinner. Drier. Less elastic. Collagen decreases. Blood flow slows. What used to be a minor scrape can quickly become a significant wound.
That is why elderly wound care tips are not simply “regular wound care done gently.” They require a different level of awareness.
The Journal of the American Geriatrics Society estimates that up to 1.5 million older adults experience skin tears each year in the United States. Many of these injuries happen during routine dressing removal. Small adjustments prevent major setbacks.
1. Protect The Skin Around The Wound
The skin surrounding a wound, often called peri-wound skin, needs just as much attention as the wound itself.
Use a barrier film spray or protective cream on the surrounding area before applying adhesive. This creates a protective layer so tape sticks to the barrier, not directly to fragile skin.
Avoid placing adhesive directly on thin or irritated areas when possible. This simple step dramatically improves home wound care safety for seniors.
2. Choose Skin-Friendly Dressings
Standard athletic tape or plastic bandages can cause “skin stripping” during removal.
Instead, consider:
- Silicone-bordered dressings
- Soft foam dressings
- Tubular bandages for limbs
Remove adhesive slowly and in the direction of hair growth. Never rip it off quickly, even if it feels faster. In elderly wound care tips, patience prevents injury.
3. Maintain Skin Hydration
Dry skin cracks more easily. Encourage regular hydration. Apply fragrance-free moisturizers to intact skin areas, not directly inside the wound.
Nutrition also plays a role. Older adults often consume less protein than needed, which slows tissue repair. Protein, Vitamin C, zinc, and adequate fluids are critical for recovery.
Preventing wound infection is easier when the immune system is supported nutritionally.
4. Keep The Room Warm During Dressing Changes
Older adults lose body heat quickly. When the room is cold, wound cells function less efficiently. Keeping the environment warm during dressing changes at home protects circulation and comfort.
Small environmental factors matter more than most caregivers realize.
5. Inspect Hidden Areas Daily
Skin tears and pressure areas often develop in overlooked spots:
- Behind the ears
- Between toes
- Under abdominal folds
- Along the tailbone
Daily inspection helps detect early breakdown before it progresses. Early detection is one of the most powerful wound care tips for caregivers.
One of the most overlooked issues is shear injury. When a patient is pulled up in bed, the skin may stay in place while underlying tissue shifts. This internal stress can cause breakdown even before redness appears.
Always lift, never drag. Elderly wound care tips are about prevention as much as treatment. The fewer injuries that occur, the fewer wounds you need to manage.
How To Prevent Pressure Sores Before They Start
Pressure sores do not appear overnight. They develop quietly when skin and tissue are exposed to constant pressure, friction, or moisture. For caregivers, prevention is far easier than treatment, but only when the right habits are in place. Pressure sore prevention is about protecting blood flow and skin integrity every day.
1. Understand Where Pressure Sores Usually Form
Pressure sores develop most often over bony areas where padding is limited.
Common locations include:
- Heels and ankles
- Tailbone and hips
- Elbows and shoulders
- Back of the head and ears
Checking these areas daily helps catch early changes before the skin breaks down.
2. Reposition Regularly To Restore Blood Flow
When pressure stays in one spot, blood flow is restricted.
For bed-bound individuals, repositioning every two hours helps restore circulation. For those who use wheelchairs, shifting weight every 15 to 30 minutes reduces tissue stress. Consistent movement is one of the most effective prevention tools available.
3. Avoid Friction And Shearing During Movement
Skin can be damaged without an open wound.
Dragging a person across sheets can cause the skin to stick while deeper tissue moves, leading to internal injury. Always lift rather than slide when repositioning. Using draw sheets or assistance devices reduces this risk significantly.
4. Keep Skin Clean, Dry, And Protected
Moisture weakens the skin barrier.
Sweat, drainage, or incontinence increases the risk of breakdown. Gently cleansing the skin and keeping it dry helps maintain strength. Protective barrier products can be applied to surrounding skin to reduce irritation.
5. Use Support Surfaces When Needed
Mattresses and cushions matter. Pressure-relieving mattresses, heel protectors, and seat cushions help distribute weight more evenly. These tools reduce stress on vulnerable areas and support long-term skin health when mobility is limited.
6. Watch For Early Warning Signs
Pressure sores begin with subtle changes.
Look for:
- Redness that does not fade when pressed
- Warmth or firmness in the skin
- Discomfort or tenderness
Early signs mean it is time to adjust positioning and care, not wait for skin to open.
When Prevention Needs Professional Guidance
If redness persists or skin changes worsen, early wound care intervention can prevent progression.
At Inspiring Minds Wound Care, our wound care specialists help families identify risk areas, adjust routines, and prevent pressure sores before they become painful wounds.
How To Recognize The Early Signs Of Wound Infection
Infection rarely starts loudly. More often, it shows up as small changes that are easy to dismiss. For caregivers, learning to recognize these early signs can mean the difference between simple treatment and a hospital visit.
Not every change means infection, but patterns matter.
1. Watch For Changes That Worsen Instead Of Improve
Some redness and warmth are normal during healing. What is not normal is when these signs increase over time.
Be cautious if you notice:
- Redness spreading beyond the wound edges
- Swelling that continues to grow
- Pain that worsens instead of easing
Healing should trend forward, not backward.
2. Pay Attention To Drainage And Odor
Drainage offers important clues.
Clear or lightly tinted fluid can be normal. Thick, cloudy, green, or yellow drainage is not. A strong or foul odor that remains after cleaning is often an early sign of bacterial growth, even before other symptoms appear.
3. Feel The Skin, Not Just Look At It
Touch can reveal problems before they are visible.
Skin that feels unusually hot, firm, or tender compared to surrounding areas may indicate infection or inflammation. Comparing both sides of the body can help identify subtle differences.
4. Notice Changes In Overall Health Or Behavior
In older adults, infection does not always present with a fever.
Watch for:
- Sudden confusion or fatigue
- Loss of appetite
- General feeling of being unwell
These changes can be early warning signs that the body is responding to infection.
5. Use Simple Tools To Track Progress
A practical caregiver technique is to lightly outline redness with a skin-safe marker.
If redness moves beyond the outline over time, this provides clear evidence that the issue is spreading. Taking photos every few days can also help track changes and support conversations with healthcare providers.
When To Call A Wound Specialist
Caring for wounds at home is possible. But knowing your limits is part of responsible caregiving.
Calling for professional help is not failure. It is smart decision-making.
Some wounds need more than good hygiene and careful dressing changes at home. They need advanced evaluation, specialized therapies, and clinical expertise.
Here is when escalation becomes necessary.
1. The Wound Is Not Getting Smaller
A healthy wound should show gradual improvement.
If there is no noticeable reduction in size after two weeks, or if the wound appears unchanged for several dressing cycles, it is time to seek evaluation.
One of the most important wound care tips is this. Healing should move forward, not stay stuck.
A wound that stalls for four to six weeks is considered chronic and requires structured care.
2. The Wound Is Deep Or Exposing Tissue
If you can see:
- Yellow or gray tissue that does not wash away
- Muscle
- Tendon
- Bone
This is beyond basic home care.
Advanced treatment may involve debridement, specialized dressings, or other medical therapies that are not available in a home setting.
This is when to call a wound specialist without delay.
3. Repeated Infections Or Persistent Drainage
If infection symptoms return after treatment, or if drainage remains heavy despite proper hygiene, deeper issues may be present.
Underlying circulation problems, diabetes management issues, or biofilm formation can prevent full healing.
Professional evaluation identifies and removes those barriers.
4. The Patient Has Diabetes Or Circulation Issues
Individuals with diabetes or vascular disease should seek earlier consultation.
Small wounds can escalate quickly in these populations. Early specialist involvement reduces the risk of complications, including hospitalization or amputation.
Clinical research shows that early intervention by wound specialists significantly lowers amputation risk in diabetic patients.
Waiting increases risk. Early care reduces it.
5.You Feel Unsure Or Overwhelmed
This point is often overlooked.
If you are uncertain about the wound’s progress, if something feels different, or if you simply lack confidence in your approach, that is reason enough to call.
One of the most practical wound care tips is knowing when professional guidance will prevent long-term problems.
Support Healing With Expert Guidance
Caring for a wound at home is a responsibility that requires attention, patience, and consistency. By applying structured wound care tips, maintaining hygiene, performing careful dressing changes at home, and watching closely for signs of wound infection, you create a safer environment for healing.
At Inspiring Minds Wound Care, our experienced clinical team provides advanced treatment plans, evidence-based therapies, and personalized support for families navigating wound recovery. We combine years of hands-on experience with structured clinical protocols to ensure wounds heal safely and efficiently.
FAQs About Wound Care Tips For Caregivers
How often should I change a wound dressing at home?
The frequency of dressing changes at home depends on the amount of drainage and the type of wound. If the bandage becomes soaked, loose, or dirty, it should be changed immediately. For stable wounds with minimal drainage, once daily or every other day is common. Always follow medical guidance if provided.
What is the safest way to clean a wound at home?
For safe home wound care safety, use room-temperature sterile saline to gently rinse the wound. Avoid scrubbing aggressively. Do not use hydrogen peroxide or alcohol unless directed by a healthcare provider, as they can damage healthy tissue. Clean in a circular motion from the center outward.
What are early signs of wound infection I should watch for?
Early signs of wound infection include spreading redness around the wound, warmth, swelling, thick yellow or green drainage, foul odor, and increasing pain. You may also notice delayed healing. Fever, chills, or sudden confusion in elderly patients are serious warning signs and require immediate medical evaluation.
What are the most important elderly wound care tips?
The most important elderly wound care tips focus on protecting fragile, thinning skin. Use gentle, silicone-based dressings when possible and remove adhesives slowly to prevent skin tears. Keep the skin clean and moisturized, support proper nutrition and hydration, and inspect common pressure areas daily to help prevent breakdown and infection.
How can I prevent pressure sores at home?
Pressure sore prevention requires repositioning every two hours for bed-bound patients and encouraging weight shifts every 15 to 30 minutes for wheelchair users. Keep skin clean and dry, use supportive cushions, and inspect bony areas daily for redness.