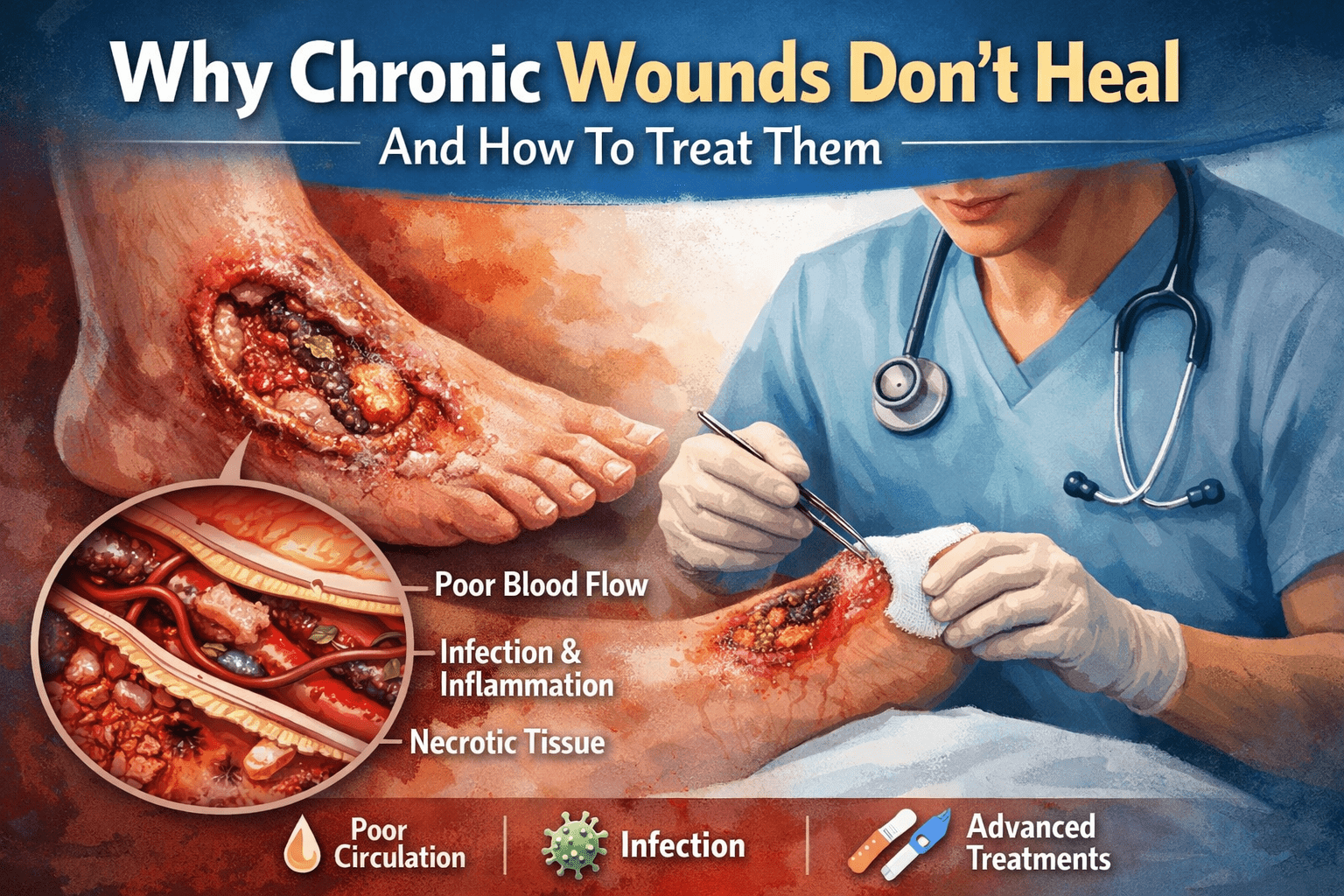
A small cut. A scraped knee. A surgical incision. It all looks simple on the surface. But beneath that bandage, your body is running a highly organized repair program. The stages of wound healing follow a precise biological sequence that decides whether your wound heals smoothly or turns into a lingering problem.
Have you ever wondered why some wounds heal in days while others drag on for weeks or months? Or why a minor sore in someone with diabetes can suddenly become serious?
In the United States, chronic wounds affect an estimated 10.5 million Medicare beneficiaries each year, roughly one in six patients, according to a 2025 wound care compendium published by Mary Ann Liebert’s journal Advances in Wound Care. That number alone tells us something important. Healing is not always automatic.
When the normal wound healing stages are disrupted, recovery slows down. Infection risk increases. Tissue breaks down instead of rebuilding.
That is exactly why understanding the process and consulting wound care specialists become essential.
At Inspiring Minds Wound Care, we guide patients through every phase of wound care with evidence-based wound treatment and personalized care in Ohio.
In this article, we will break down the complete stages of wound healing, explain what happens during each phase, and show you when it is time to move from home care to expert-level chronic wound care.
“Inspiring Minds Wound Care provides personalized, stage-focused wound treatment that helps patients heal safely at home, avoid complications, and regain comfort with confidence.”
What Is A Wound And Why Healing Fails Sometimes
A wound is any break in the skin or underlying tissue. It can be small like a paper cut. It can be deep like a surgical incision. It can even develop slowly, without you noticing at first.
The body is built to repair these injuries through the stages of wound healing. Most minor wounds move through the normal wound healing stages without help. But not all wounds behave the same way.
Healing fails when the body cannot complete its repair process properly. And when that happens, a simple injury can turn into a long-term health issue.
Let’s first understand the types of wounds. Because not every wound starts the same, and not every wound needs the same level of care.
Understanding The Different Types Of Wounds
1. Acute Wounds
Acute wounds happen suddenly. They are usually caused by trauma or surgery.
Examples include:
- Cuts and lacerations
- Scrapes and abrasions
- Surgical incisions
- Minor burns
These wounds typically follow a predictable wound healing timeline. With proper cleaning and protection, they move through the repair process smoothly.
If everything works as it should, healing is steady and visible week by week. But even acute wounds can stall if infection, poor circulation, or pressure interferes.
2. Chronic Wounds
Chronic wounds are different. They do not progress normally through the wound healing stages. Instead of closing, they linger.
A wound is generally considered chronic if it does not improve within four weeks.
Common chronic wounds include:
- Diabetic foot ulcers
- Pressure injuries, sometimes called bedsores
- Venous leg ulcers
- Arterial ulcers
These wounds often require structured chronic wound care because something is blocking the natural healing process. It is not about applying more bandages. It is about identifying the root cause.
3. Surgical Wounds
Surgical wounds are planned incisions made during medical procedures. They usually heal well because they are clean and controlled.
However, healing can fail if:
- Infection develops
- Sutures reopen
- Blood flow is limited
- Underlying conditions interfere
When surgical wounds do not follow the expected wound healing timeline, early evaluation prevents complications.
4. Pressure Injuries
Pressure injuries develop slowly due to constant pressure on one area of the body.
They commonly appear on:
- Heels
- Hips
- Tailbone
- Elbows
These wounds form when blood supply is reduced over time. Without enough oxygen, tissue begins to break down.
Pressure injuries often require professional chronic wound care, especially if deeper layers are affected.
5. Diabetic Wounds
Diabetes changes the healing equation.
High blood sugar can:
- Damage small blood vessels
- Reduce circulation
- Slow immune response
- Cause nerve damage, which reduces pain awareness
This is why even a small blister on the foot can turn serious. Diabetic wounds frequently stall within the stages of wound healing and require careful monitoring.
Early treatment makes a major difference.
6. Traumatic Wounds
These result from accidents or injuries.
Examples include:
- Puncture wounds
- Crush injuries
- Deep lacerations
Traumatic wounds may damage tissue beneath the surface. Even if the skin looks small on the outside, deeper layers can be affected.
These wounds need proper assessment to ensure they move forward in the normal wound healing stages.
Why Healing Fails Even When You Think You Are Doing Everything Right
Here is the frustrating part. Many people believe they are caring for their wounds properly.
They clean it. They cover it. They wait.
But healing is not just about what happens on the surface.
Common reasons why wounds won’t heal:
- Poor Circulation: Without oxygen-rich blood, tissue cannot rebuild.
- Uncontrolled Diabetes: Elevated glucose slows immune defense and collagen production.
- Infection: Even low-level bacterial presence can freeze progress in the inflammation phase.
- Excess Moisture Or Dryness: Wounds need balance. Too wet or too dry both delay repair.
- Repeated Pressure Or Friction: Constant rubbing damages fragile new tissue.
- Poor Nutrition: Your body cannot rebuild tissue without protein and essential nutrients.
When one or more of these factors exist, the wound healing timeline stretches longer than expected. That delay increases the risk of complications.
And here is something most people do not realize. If a wound does not reduce in size within two to four weeks, it is unlikely to close without targeted intervention. That is when professional evaluation becomes important.
Need Professional Wound Care At Home?
Get the right support at the right time. Explore our mobile wound care services or speak with a specialist today to help your wound heal safely and confidently.
How The Wound Healing Process Works Inside The Body
Wound healing is not random, and it is not passive. The body follows a built-in repair system that activates the moment the skin is damaged. Whether a wound is small or complex, the process always follows the same core pattern. What changes is how smoothly each phase moves forward.
Here is where most people get stuck. From the outside, wounds can look similar. From the inside, they behave very differently. Healing depends on timing, blood flow, immune response, and how well each stage supports the next one. When even one part slows down, the entire process can stall.
This is not just a clinical issue. It is a growing global concern. According to Towards Healthcare, the global advanced wound care market was valued at USD 11.28 billion in 2024 and is projected to reach USD 18.04 billion by 2034, growing steadily as more wounds fail to progress through normal healing stages. Source to add later: Towards Healthcare via GlobeNewswire, April 25, 2025.
That growth tells an important story. More wounds are becoming complex, slower to heal, and harder to manage without structured, stage-based care.
This is why effective wound care is not about rushing closure or waiting for a scab to form. It is about guiding the body through each healing phase in the correct order and at the right pace.
At a basic level, the wound healing process works like this:
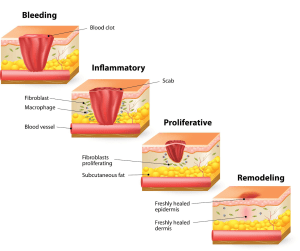
- First, the body stops the bleeding and protects the area
- Then, it cleans the wound by removing damaged tissue and bacteria
- Next, it rebuilds new tissue and blood vessels
- Finally, it strengthens and remodels the skin over time
These stages overlap, but they must happen in sequence. Skipping ahead does not speed healing. It usually creates setbacks.
This is where many home-managed wounds struggle. People focus on what they can see, redness, scabbing, or closure, but healing depends just as much on what is happening beneath the surface.
At Inspiring Minds Wound Care, we evaluate wounds based on the healing stage the body is actually in, not just how the wound looks that day. This stage-focused approach helps prevent wounds from stalling, reopening, or becoming infected.
The Four Stages Of Wound Healing: Explained Step By Step
Every wound heals through the same four stages. What changes is how long each stage lasts and whether the body is able to move forward without interruption. Understanding these stages helps set realistic expectations and prevents panic when healing does not look perfect every day.
Each stage below includes what is happening inside the body, what is normal, and when extra care may be needed.
1. Stage One: Hemostasis, When The Body Stops The Bleeding
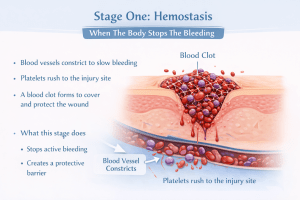
Hemostasis begins immediately after a wound occurs. The body’s first priority is control.
Blood vessels constrict to slow blood flow. Platelets gather at the injury site and form a clot. This clot acts as a temporary seal and protects the wound from further damage or contamination.
What this stage does
- Stops active bleeding
- Creates a protective barrier
- Signals the body to begin repair
What is normal
- Mild oozing that stops quickly
- Formation of a clot or scab
- Slight tenderness around the area
What can interfere
- Blood thinning medications
- Repeated trauma or reopening
- Poor clotting ability
If bleeding continues or the wound keeps reopening, the healing process cannot move forward. This is often the first sign that professional wound assessment is needed.
2. Stage Two: Inflammation, When The Wound Is Cleaned
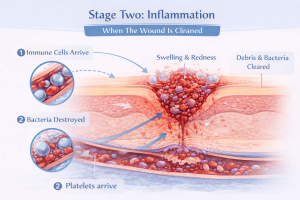
This is the stage most people misunderstand. Inflammation is not a problem. It is the body’s cleanup phase. White blood cells move in to remove bacteria, damaged tissue, and debris. Blood flow increases to deliver oxygen and nutrients.
What this stage does
- Clears bacteria and dead tissue
- Prevents infection
- Prepares the wound for rebuilding
What is normal
- Redness and warmth
- Mild swelling
- Tenderness or soreness
What is not normal
- Increasing pain after several days
- Thick drainage or foul odor
- Spreading redness beyond the wound
Inflammation should calm down within a few days. When it does not, the wound can become stuck. Many chronic wounds stall at this stage, which is why inflammation control is a major focus of advanced wound care.
3. Stage Three: Proliferation, When New Tissue Grows
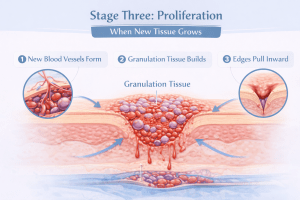
This is the rebuilding phase. New tissue forms from the bottom up. Blood vessels regrow. Collagen is produced to strengthen the wound bed. The wound begins to shrink as edges pull inward.
What this stage does
- Builds granulation tissue
- Restores blood supply
- Fills the wound depth
What is normal
- Pink or red tissue that looks moist
- Gradual reduction in wound size
- Less pain than earlier stages
What can slow progress
- Poor circulation
- Pressure on the wound
- Inadequate nutrition or hydration
This stage requires protection and balance. Too much moisture causes breakdown. Too little dries tissue out. Proper dressing selection matters more here than at any other stage.
4. Stage Four: Maturation, When Strength Returns
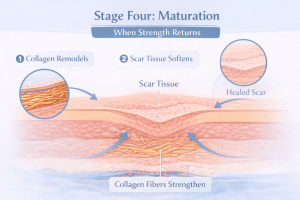
Maturation is the longest stage and the easiest to underestimate.
The wound may look closed, but healing is still ongoing beneath the surface. Collagen fibers reorganize, scars soften, and tensile strength slowly increases.
What this stage does
- Strengthens repaired tissue
- Improves flexibility
- Reduces visible scarring
What is normal
- Color changes in the scar
- Tightness that improves over time
- Gradual return of function
Important to know
- Healed skin is never as strong as uninjured skin
- Protection is still necessary
- Reinjury can reopen the wound
This stage can last months. Ongoing care and monitoring reduce the risk of recurrence, especially for patients with diabetes, mobility issues, or circulation problems.
Why Wounds Get Stuck Between Stages
Most slow-healing wounds are not failing. They are paused.
Common reasons include:
- Pressure that cuts off blood flow
- Infection that prolongs inflammation
- Incorrect dressing use
- Missed early warning signs
This is why stage-based evaluation matters. Treating a wound without identifying its healing stage is like fixing a roof without knowing where the leak is.
At Inspiring Minds Wound Care, we assess wounds by stage, depth, and underlying risk factors. That approach helps move healing forward instead of repeating the same care that has already failed.
When A Wound Becomes Chronic
A wound that does not show meaningful improvement within four weeks is often considered chronic. At this point, the normal wound healing stages are disrupted, and the body struggles to move forward on its own.
Chronic wounds are not rare, and they are not a failure of effort. They usually signal that something beneath the surface is blocking progress.
Common examples include:
- Diabetic foot ulcers
- Pressure injuries
- Venous leg ulcers
These wounds require targeted chronic wound care, not just repeated dressing changes. Without addressing the underlying cause, healing remains stalled.
Warning signs a wound may be chronic:
- No visible size reduction after two to four weeks
- Repeated reopening after partial closure
- Persistent or increasing drainage
- Darkened, thickened, or dead tissue
Waiting rarely solves chronic wounds. Early evaluation shortens recovery time, lowers infection risk, and helps prevent long-term complications.
Practical Steps To Support Each Healing Stage
Wound healing does not happen automatically. It needs the right conditions at the right time. While every wound is different, these fundamentals support healing across all stages.
1. Keep The Wound Clean
Use gentle cleansing methods. Harsh chemicals can damage healthy tissue and delay repair.
2. Protect The Area
Appropriate coverage reduces contamination and supports moisture balance. Leaving wounds exposed often slows healing.
3. Manage Swelling
Elevation and pressure relief improve circulation, especially for wounds on the legs or feet.
4. Support Nutrition
Protein, hydration, and balanced nutrition directly affect tissue repair. Healing demands energy.
5. Monitor Progress Weekly
Improvement should be visible over time. Even small changes matter.
If the wound healing timeline stalls, professional care prevents escalation. Sometimes the smartest move is not another home remedy. It is an expert evaluation.
When To Seek Professional Wound Care
Knowing when to ask for help is not a weakness. It is prevention.
Professional wound care should be considered when:
- A wound shows little or no improvement after two to four weeks
- Pain, redness, or drainage increases instead of decreases
- The wound repeatedly reopens
- There is a history of diabetes, poor circulation, or limited mobility
- Daily wound care feels confusing or overwhelming
Wounds that linger tend to worsen quietly. What starts as slow healing can turn into infection, tissue damage, or hospitalization if left unmanaged. Early, stage-based intervention often means fewer complications, faster recovery, and less disruption to daily life.
This is where experienced wound care specialists make the difference, by guiding the body through healing the way it was designed to work.
Heal With Inspiring Minds Wound Care
The body follows a clear system during the stages of wound healing. When that system works, recovery feels natural. When it stalls, complications grow quietly.
Understanding the process helps you recognize when healing is normal and when it is not.
At Inspiring Minds Wound Care, we specialize in advanced chronic wound care, using evidence-based treatment plans, certified wound care specialists, and years of clinical expertise to guide patients safely through every phase of healing.
We evaluate circulation, infection risk, pressure factors, and overall health to support a healthy wound healing timeline. Our goal is simple. Close wounds safely. Reduce complications. Restore quality of life.
Early action protects your health. Healing works best when the right care meets the right stage at the right time.
Frequently Asked Questions
How long does each stage of wound healing last?
Wound healing has four stages. Hemostasis begins within minutes to control bleeding. The inflammatory stage usually lasts 2 to 5 days. The proliferative stage can take several days to a few weeks as new tissue forms. The maturation stage may continue for several months while the wound strengthens and fully remodels.
When should I worry about a wound not healing?
You should be concerned about a wound not healing if there is no visible improvement within 10 to 14 days or if the wound appears larger, deeper, or unchanged after four weeks. Ongoing redness, swelling, drainage, or increasing pain may also indicate delayed healing and require professional wound care evaluation.
Can diabetes slow down wound healing?
Yes, diabetes can significantly slow down wound healing. High blood sugar levels reduce proper circulation and weaken immune function, making it harder for the body to repair damaged tissue. This delay increases the risk of infection and chronic wounds, especially in the feet and lower legs, requiring careful monitoring and professional wound care.
Should wounds be kept covered or left open to heal?
Most wounds heal more effectively when properly covered with the right dressing. Appropriate wound dressings protect against bacteria, maintain a balanced moist environment, and support healthy tissue growth during the healing stages. Leaving a wound open can dry out new tissue, delay the proliferative phase, and increase the risk of contamination or infection.
When should professional wound care be considered?
Professional care should be sought if healing stalls, pain or drainage increases, or care feels difficult to manage at home. Early intervention often prevents infection, shortens recovery time, and reduces the risk of complications, especially for complex or recurring wounds.